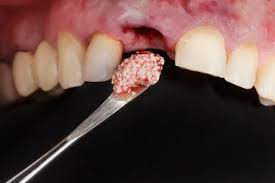
Why Bone Grafting?
Dental implants are an excellent way to replace missing teeth — but not everyone qualifies as a candidate for implant dentistry. Tooth loss from periodontal disease or other dental conditions may cause the jaw bone to weaken, and the resulting bone loss will lessen the possibility of the patient being able to support a dental implant or other dental appliance.
In such a case, a procedure called bone grafting is often used to add bone to the jaw. Bone is taken from another area in the body and transplanted to the jaw bone to increase its mass.
Once the grafted bone fuses to the jaw bone, a dental implant can be placed, with greater chances for success. Bone grafting is also used to improve bone deterioration caused by dentures, oral cancer, dental deformities or a tooth extraction.
Explore Your Resources
During the bone grafting procedure, bone is taken from any one of a number of locations in the body. The most convenient areas for bone grafting are your chin or the back part of your lower jaw. If bone is needed to support multiple dental implants, the hip or shin may be used to provide a larger amount of bone. Regardless, any area that provides a significant amount of bone marrow is your best bet for successful healing.
Bone marrow pulled directly from the patient is most recommended by dentists for bone grafting materials. That’s because your own bone marrow contains live cells that help continue bone growth and speed up the healing process. But if there’s not enough bone available or if you aren’t comfortable having bone removed, bone marrow may be taken from human cadavers or cows. Synthetic materials may also be used.
Scalpel, Please
Bone graft dental surgery does not have to be extensive, yet it depends on the situation. When a single tooth implant is needed and bone is donated from the chin or jaw, the procedure can be performed in a dental office with local anesthesia. But if multiple implants are planned and a greater mass of bone is removed from another area of the body, a hospital stay may be required.
During this type of oral surgery, the dentist will numb both the area where bone is being extracted and the part of the jaw that is expecting the graft. After cutting open the transplant area and assessing how much bone is needed, the dentist makes an incision in the gums to locate bone in the jaw or chin. Bone is extracted, and the hole is filled for support. The healthy bone is then secured to the deteriorating bone by screws, enabling it to fuse together as it heals.
Guided bone regeneration, or GBR, often goes hand-in-hand with bone grafting. During GBR, both areas are covered with a membrane to protect the bone during the healing process. Because a membrane is made up of tissue, it encourages bone growth. The membrane also acts as a barrier from outside elements, helps prevent infection and keeps scar tissue from forming.
Post-Operative Details
Following the bone graft surgery, it’s important to adhere to your dentist’s post-operative instructions to prevent the bone graft from failing. Your dentist can prescribe you pain medication and an antibacterial mouthwash to keep the area clean. If all goes well, the screws can be removed once healing is complete, which is usually in about six to nine months.
Bone grafting and guided tissue regeneration are often necessary for those who suffer from bone loss. Without appropriate dental treatment to rebuild the bone, the jaw will continue to deteriorate, leading to further tooth loss. And in the case of extreme bone loss, it will not only be incredibly difficult to support a denture, but the structure of the face will start to collapse, leading to premature aging.